Glaucoma Treatment in Hyderabad — Eye Drops, Laser Surgery
Glaucoma is called the “silent thief of sight” — it causes permanent vision loss before most patients realise anything is wrong. At SurgiPartner Hyderabad, our specialist glaucoma team detects, monitors, and treats all types of glaucoma using a stepwise, evidence-based approach — from prescription eye drops and selective laser trabeculoplasty to advanced filtration surgery.


What Is Glaucoma?
Glaucoma is a group of eye diseases characterised by progressive damage to the optic nerve — the nerve that transmits visual information from the eye to the brain. In most cases, this damage is caused by elevated intraocular pressure (IOP), the fluid pressure inside the eye. As the optic nerve fibres are progressively lost, the visual field gradually narrows, beginning with peripheral vision and ultimately threatening central vision and total blindness if left untreated.
Glaucoma is the second leading cause of blindness worldwide and the leading cause of irreversible blindness. In India, an estimated 12 million people have glaucoma, with over 1.2 million completely blind from the condition. Most tragically, approximately 90% of glaucoma-related blindness is preventable with early detection and consistent treatment.
The critical challenge is that the most common form of glaucoma — primary open-angle glaucoma — causes no pain and no visible changes until significant, permanent vision loss has already occurred. By the time patients notice symptoms, they may have lost 30–40% of their optic nerve fibres irreversibly. This is why regular glaucoma screening is essential, particularly for high-risk individuals.
Types of Glaucoma — Understanding Your Diagnosis
Primary Open-Angle Glaucoma (POAG)
The most common type, accounting for 70–80% of all glaucoma cases in India. The drainage angle of the eye remains open, but the trabecular meshwork (the eye’s drainage system) becomes progressively less efficient, causing a gradual rise in IOP. The condition is completely painless and asymptomatic until advanced stages. POAG is strongly associated with increasing age, elevated IOP, family history, and African ancestry.
Primary Angle-Closure Glaucoma (PACG)
More common in Asian populations, including South Indians. The drainage angle between the iris and cornea narrows or closes suddenly or gradually, blocking aqueous fluid outflow and causing a rapid or chronic rise in IOP. Acute angle-closure glaucoma presents as a painful emergency with severe eye pain, headache, nausea, blurred vision, and coloured halos around lights — requiring immediate treatment.
Normal-Tension Glaucoma (NTG)
Optic nerve damage occurs despite IOP remaining within statistically normal ranges. The exact mechanism is not fully understood but is believed to involve reduced blood flow to the optic nerve and optic nerve vulnerability. NTG requires careful management and close follow-up.
Secondary Glaucoma
Glaucoma resulting from another eye condition or systemic disease — including pseudoexfoliation glaucoma, pigmentary glaucoma, uveitic glaucoma, neovascular glaucoma (commonly associated with diabetic retinopathy), and steroid-induced glaucoma. Treatment addresses both the primary condition and the elevated IOP.
Congenital / Developmental Glaucoma
Present from birth or developing in early childhood due to abnormal development of the eye’s drainage system. Characterised by enlarged eyes (buphthalmos), light sensitivity, excessive tearing, and corneal cloudiness. Requires early surgical intervention.
Risk Factors for Glaucoma — Who Should Be Screened?
You have a significantly higher risk of developing glaucoma if you have any of the following:
- 1. Age over 40 — risk increases substantially with each decade
- 2. Family history of glaucoma (first-degree relatives)
- 3. High myopia (short-sightedness) or high hyperopia
- 4. Elevated intraocular pressure (IOP) — even without glaucoma (ocular hypertension)
- 5. Diabetes mellitus or systemic hypertension
- 6. Long-term use of corticosteroids (eye drops, tablets, or inhalers)
- 7. Prior eye injuries or eye surgeries
- 8. Thin central corneal thickness
- 9. Migraine or Raynaud’s phenomenon (vascular factors affecting optic nerve)
If you have two or more risk factors, annual glaucoma screening at SurgiPartner Hyderabad is strongly recommended.
Call +91 9030053009 to schedule your evaluation.
Glaucoma Diagnosis — What Tests Are Performed?
Accurate glaucoma diagnosis requires a comprehensive evaluation rather than IOP measurement alone. SurgiPartner’s glaucoma specialists use all diagnostic modalities:
| Diagnostic Test | What It Measures | Clinical Significance |
|---|---|---|
| Tonometry (IOP Measurement) | Intraocular pressure | Elevated IOP (>21 mmHg) is a key risk factor; normal IOP does not exclude glaucoma |
| Gonioscopy | Drainage angle structure | Differentiates open-angle from angle-closure glaucoma — essential for treatment planning |
| Optic Disc Examination | Optic nerve appearance | Cupping (C/D ratio), pallor, and disc haemorrhages indicate glaucomatous damage |
| Visual Field Test (Perimetry) | Functional vision loss | Maps areas of vision loss; monitors disease progression over time |
| OCT (Optical Coherence Tomography) | Retinal nerve fibre layer thickness | Detects structural damage before functional loss; most sensitive early detection tool |
| Pachymetry (Corneal Thickness) | Central corneal thickness | Affects IOP reading accuracy; thin corneas are independent glaucoma risk factors |
Glaucoma Treatment — A Step-by-Step Approach
Glaucoma treatment aims to lower IOP to a level that prevents further optic nerve damage. The approach is stepwise, beginning with the least invasive option and escalating as needed. Unlike many conditions, glaucoma cannot be cured — but it can be effectively controlled to preserve existing vision for life.
Step 1: Eye Drops (Medical Management)
The first line of treatment for most glaucoma patients. Prescription eye drops lower IOP by either reducing aqueous humour production or increasing its drainage from the eye. Common drug classes include prostaglandin analogues (latanoprost, travoprost), beta-blockers (timolol), alpha-2 agonists (brimonidine), and carbonic anhydrase inhibitors (dorzolamide). Strict daily adherence is essential — missing doses allows IOP to rise and optic nerve damage to progress. SurgiPartner’s team provides detailed education and reminder systems to support long-term compliance.
Step 2: Laser Treatment
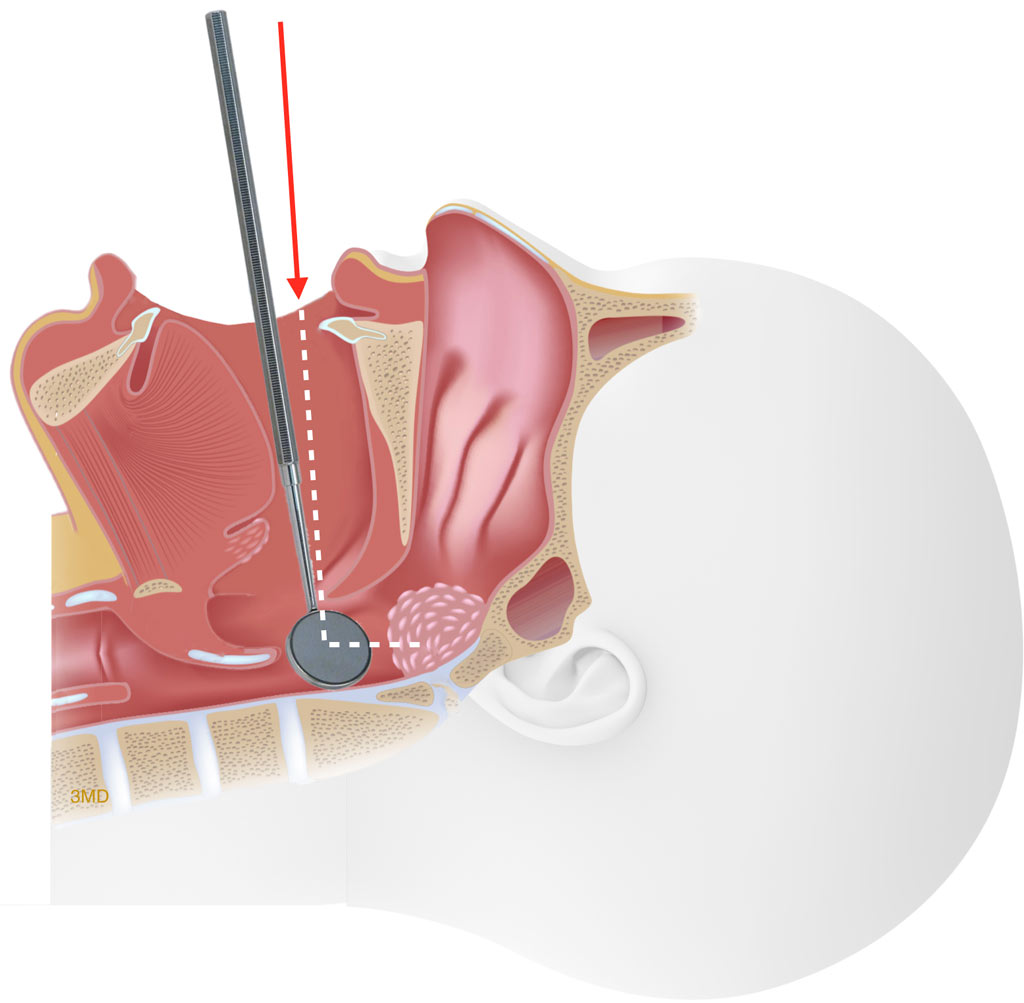
Selective Laser Trabeculoplasty (SLT) is a safe, painless 5-minute outpatient procedure that uses a low-energy laser to treat the trabecular meshwork, improving drainage and lowering IOP. SLT is effective in 70–80% of patients and can reduce or eliminate the need for daily eye drops. It can be repeated and has no adverse effects on surrounding tissue.
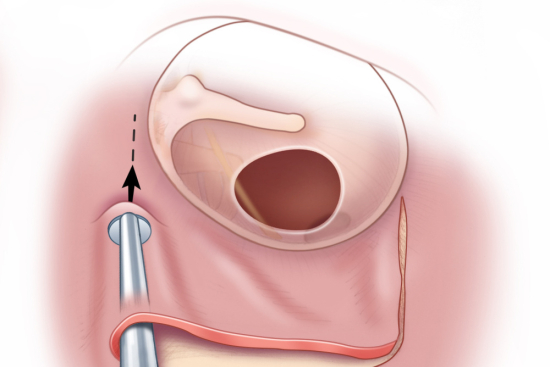
Laser Peripheral Iridotomy (LPI) is the definitive treatment for angle-closure glaucoma. A small laser hole is created in the peripheral iris, allowing aqueous fluid to bypass a blocked pupillary aperture and reach the drainage angle. LPI eliminates the risk of acute angle-closure attacks and is often performed prophylactically in the second eye when angle-closure is detected in one eye.
Step 3: Glaucoma Surgery
When eye drops and laser treatment are insufficient to control IOP, surgery creates a new drainage pathway or reduces fluid production.
Trabeculectomy (filtration surgery) creates a small flap in the sclera through which aqueous fluid drains into a subconjunctival blister (bleb). It remains the gold-standard glaucoma surgery with excellent long-term IOP control. Mitomycin-C (MMC) is often applied to reduce scarring and improve outcomes.
Glaucoma Drainage Devices (GDD) — tube shunts (Ahmed, Baerveldt) are silicone tubes that redirect aqueous fluid to a plate sutured to the eye’s surface. GDDs are particularly useful in refractory glaucoma, failed trabeculectomy, and neovascular or uveitic glaucoma.
Minimally Invasive Glaucoma Surgery (MIGS) — newer techniques such as iStent, Kahook Dual Blade, and Xen Gel Stent offer safer, more targeted IOP reduction with faster recovery, often performed simultaneously with cataract surgery in patients with mild to moderate glaucoma.
Living With Glaucoma — Long-Term Management
Glaucoma is a lifelong condition requiring consistent monitoring and treatment adherence. Key principles of long-term glaucoma management include:
- 1. Regular follow-up appointments (typically every 3–6 months) including IOP measurement, visual field testing, and OCT imaging
- 2. Consistent daily use of prescribed eye drops — never stopping without medical guidance
- 3. Informing all treating physicians about glaucoma diagnosis to avoid medications that raise IOP
- 4. Regular general health monitoring — particularly blood pressure and blood sugar, which affect optic nerve perfusion
- 5. Protective eyewear during sports and activities that risk eye trauma
- 6. Encouraging first-degree relatives (parents, siblings, children) to undergo glaucoma screening
Living With Glaucoma — Long-Term Management
Yes — family history is one of the strongest risk factors for glaucoma. First-degree relatives (parents, siblings, children) of a glaucoma patient have a 4–10 times higher risk of developing the condition compared to the general population. SurgiPartner strongly recommends that all first-degree relatives of glaucoma patients undergo comprehensive screening, ideally starting from age 40 (or earlier if other risk factors are present).
Primary open-angle glaucoma — the most common type — causes no pain whatsoever. This is precisely why it is so dangerous. Vision is lost silently. Acute angle-closure glaucoma, by contrast, presents with severe eye pain, headache, nausea, and vomiting — a painful emergency requiring immediate treatment. Chronic angle-closure glaucoma may cause mild, intermittent symptoms.
Adults over 40 with any risk factors should have a comprehensive glaucoma evaluation at least once a year. Patients already diagnosed with glaucoma typically need follow-up every 3–6 months, depending on disease severity and IOP control. SurgiPartner's glaucoma specialists create personalised monitoring schedules for each patient.
No — yoga and eye exercises do not cure or effectively treat glaucoma. Some inversional yoga poses (such as headstands) may actually temporarily raise IOP. While general physical activity and a healthy lifestyle support overall eye health, glaucoma requires specific medical treatment to lower IOP. Never delay prescribed glaucoma treatment in favour of alternative therapies.
Why Choose SurgiPartner?
Choosing SurgiPartner means choosing precision, safety, and innovation. Our approach toGlaucoma combines world-class laser systems with the expertise of highly trained ophthalmologists — ensuring every patient experiences a smooth, pain-free journey to perfect vision.
01.
Expert Ophthalmic Surgeons
Our team includes experienced specialists who have performed thousands of successful Glaucoma surgeries with exceptional outcomes.
02.
Advanced Diagnostic Technology
We use OCT scans, visual field testing, and modern tonometry for accurate evaluation.
03.
Personalized Treatment Plans
Every eye is unique — and so is our approach. We tailor each Glaucoma procedure to match your specific vision needs.
04.
Continuous Monitoring & Care
Glaucoma requires lifelong monitoring—and we stay with you at every step.
Book Your Consultation
Early diagnosis is the key to preventing vision loss.
Trust SurgiPartner’s advanced glaucoma treatment in Hyderabad to protect your eyesight.
Protect today. Preserve vision for life.
What Our Patients Say
Posted onTrustindex verifies that the original source of the review is Google. I am thoroughly impressed with the SurgiPartner model, which delivers integrated, end-to-end patient support across the healthcare continuum—from initial consultations to treatment and surgical interventions, where necessary. I recently availed their Care Buddy service for a consultation, and the experience was highly seamless, efficient, and professionally managed. The structured Care Buddy support, combined with well-aligned financial assistance processes, significantly enhances the overall patient journey. This holistic and patient-centric approach effectively streamlines access to quality healthcare, making it more efficient and convenient in today’s dynamic environment.Posted onTrustindex verifies that the original source of the review is Google. I’m really impressed with the SurgiPartner concept. They provide end-to-end patient support—from doctor consultations to treatment and even surgery when required. I personally used their Care Buddy service for a consultation, and it was a smooth and positive experience. The Care Buddy assistance, along with support in financial processes, makes healthcare much more convenient, especially in today’s fast-paced lifestyle.Posted onTrustindex verifies that the original source of the review is Google. My Brother Arun Kumar and krishna from Bangalore. We are travelled to Hyderabad for LASIK surgery, and today we successfully underwent the procedure at American Laser Eye Hospital. The surgery went very smoothly and I am feeling very good after the procedure. The hospital environment is very clean and well maintained. All the staff and doctors are very polite, supportive, and professional. A special thanks to SurgiPartner CareBuddy for guiding and helping me throughout the entire process. From the beginning till the end of the day, they were with us at every step and provided excellent support. Overall, I had a very good experience and I highly recommend American Laser Eye Hospital for LASIK surgery with SurgiPartner support.Posted onTrustindex verifies that the original source of the review is Google. Really impressed with the concept of SurgiPartner. They offer complete patient support from doctor consultation to treatment and surgery if needed. I personally took a consultation through their Care buddy, and it was a great experience. The care buddy system and help with financial processes make healthcare much easier, especially in today’s busy world.Posted onTrustindex verifies that the original source of the review is Google. My name is Arun Kumar and I am from Bangalore. I traveled to Hyderabad for LASIK surgery, and today I successfully underwent the procedure at American Laser Eye Hospital. The surgery went very smoothly and I am feeling very good after the procedure. The hospital environment is very clean and well maintained. All the staff and doctors are very polite, supportive, and professional. A special thanks to SurgiPartner CareBuddy for guiding and helping me throughout the entire process. From the beginning till the end of the day, they were with us at every step and provided excellent support. Overall, I had a very good experience and I highly recommend American Laser Eye Hospital for LASIK surgery with SurgiPartner supportPosted onTrustindex verifies that the original source of the review is Google. Thank you for the support and service provided by SurgiPartner. The overall experience was smooth and the team was very helpful.Posted onTrustindex verifies that the original source of the review is Google. Staff is very good and nice receiving. They are very humble and their response is very good. Thank youPosted onTrustindex verifies that the original source of the review is Google. I want to thank Surgipartner for all the help and support during my LASIK surgery. From the beginning till the end, the team was very proactive with follow-ups and guided me clearly through every step, which made the whole experience easy and stress-free. I would especially like to appreciate CareBuddy Raju and Coordinator Anusha for their outstanding support. They were always in touch with both the hospital staff and me, helped reduce waiting time, and made sure everything went smoothly. Their care, quick responses, and constant guidance really made a big difference. Overall, I had a very positive experience and truly appreciate the support provided by Surgipartner.Verified by TrustindexTrustindex verified badge is the Universal Symbol of Trust. Only the greatest companies can get the verified badge who has a review score above 4.5, based on customer reviews over the past 12 months. Read more
Your Personalized Path to Wellness
Follow your step-by-step guide to a successful surgery and recovery, with our expert team supporting you all the way.
Book FREE Consultation
Fill in your details and we'll call you back to confirm your slot.
Popular Diseases
Other Diseases
Get it Touch
Tell us about your problems and we’ll figure out the best treatment option for you.
Glaucoma Treatment Services Across Hyderabad
SurgiPartner offers advanced glaucoma treatment and surgery in Hyderabad through its trusted network of clinics and partner hospitals 0 bringing world-class eye care closer to you.