Knee Replacement Surgery: When You Need It, What to Expect, and Life After
You used to climb stairs without thinking about it. Now, every step up feels like a small battle.
You used to enjoy long walks with family. Now, knee pain cuts them short.
You used to sleep through the night. Now, knee pain wakes you at 2 AM.
If this sounds familiar, you might have knee arthritis. And you’re not alone. Millions of people face the same struggle.
But here’s the important part: You don’t have to live with this pain forever.
Knee replacement surgery has helped millions of people—including people in their 60s, 70s, and even 80s—return to active, pain-free lives. It’s one of the most successful orthopedic surgeries available today.
In this guide, we’ll explain when knee replacement is the right choice, what the surgery involves, what real recovery looks like, and most importantly, how your life can improve.
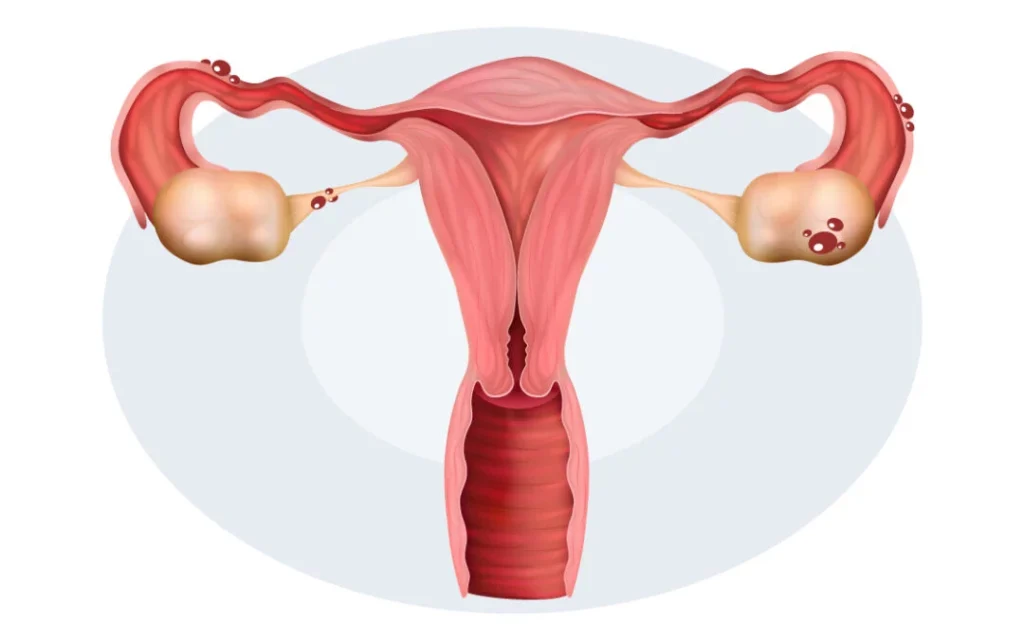
Understanding Knee Arthritis: Why Your Knee Hurts
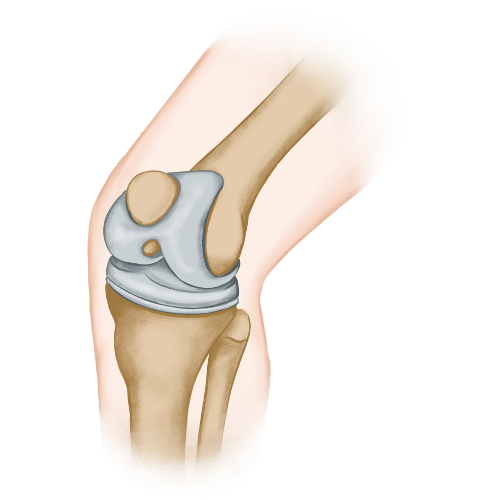
Your knee is a complex joint. The ends of your bones are covered with smooth cartilage that acts like a shock absorber and allows smooth movement. In healthy knees, this cartilage is strong and slippery. Your knee glides effortlessly. In arthritic knees, this cartilage wears away. Bone starts rubbing on bone. This causes:- 1. Pain (especially with activity or bearing weight)
- 2. Stiffness (especially in the morning)
- 3. Swelling (from inflammation)
- 4. Instability (knee feels weak or “gives way”)
- 5. Reduced mobility (you can’t do activities you love)
Types of Knee Arthritis
1. Osteoarthritis (Most Common)- a. Wear-and-tear arthritis
- b. Develops over years
- c. More common after age 50
- d. Caused by age, weight, previous injury, or genetics
- 1. Autoimmune condition
- 2. Can affect younger people
- 3. Develops more suddenly
- 4. Affects multiple joints
- a. Develops after knee injury (ACL tear, meniscus damage, fracture)
- b. Can occur at any age
- c. Often develops 10-20 years after the initial injury
When is Knee Replacement the Right Choice?
Knee replacement isn’t about convenience. It’s about quality of life. You’re a good candidate for knee replacement if:A. You Have Significant Pain
- 1. Pain with daily activities (stairs, walking, sitting down)
- 2. Pain that doesn’t respond to medications
- 3. Pain that affects your sleep
- 4. Pain that’s limited your activities for months
B. Conservative Treatments Haven’t Worked
You’ve tried:- 1. Anti-inflammatory medications
- 2. Weight management
- 3. Physical therapy
- 4. Injections (cortisone, hyaluronic acid)
- 5. Assistive devices (cane, walker, knee brace)
C. The Pain is Affecting Your Life
- 1. Can’t do activities you care about
- 2. Isolated because you can’t socialize
- 3. Depressed because of limitation
- 4. Dependent on family for basic tasks
- 5. Sleep disrupted nightly
D. Your Knee X-rays Show Advanced Arthritis
- 1. Advanced cartilage loss visible on imaging
- 2. Bone-on-bone rubbing
- 3. Significant joint space narrowing
E. You’re Generally Healthy
- 1. No uncontrolled heart disease
- 2. No active infections
- 3. No severe medical conditions that make surgery risky
- 4. Age is not a limiting factor (people in their 80s have successful knee replacements)
Conservative Treatments: What to Try First
Before jumping to surgery, most doctors recommend:1. Medications
- a. Over-the-counter pain relievers (ibuprofen, naproxen)
- b. Prescription anti-inflammatory medications
- c. Topical pain creams
- d. Injections: Cortisone (temporary relief) or hyaluronic acid (lubrication)
2. Weight Management
Every extra kilogram adds pressure to your knees. Losing even 5-10 kg can significantly reduce pain.3. Physical Therapy
Strengthening the muscles around your knee reduces stress on the joint. Quadriceps and hamstring strength is crucial.4. Activity Modification
- a. Avoid high-impact activities (running, jumping)
- b. Prefer low-impact activities (swimming, cycling, walking)
- c. Use assistive devices (cane, walker, knee brace)
5. Lifestyle Adjustments
- a. Warm showers to reduce morning stiffness
- b. Ice after activities to reduce inflammation
- c. Elevation to manage swelling
- d. Heat therapy for stiffness
Knee Replacement Surgery: The Step-by-Step Process
What Gets Replaced?
Your surgeon removes the damaged cartilage and bone from:- a. The end of your thighbone (femur)
- b. The top of your shinbone (tibia)
- c. The back of your kneecap (patella) – sometimes
The Actual Surgery (1.5-2 hours)
Before Surgery- a. Spinal or general anesthesia
- b. Your leg is cleaned and prepped
- c. Surgeons position your leg for optimal access
- 1. Incision – A 15-20 cm incision along the front of your knee (not as scary as it sounds; your surgeon is experienced)
- 2. Damage Assessment – Surgeon evaluates cartilage damage and underlying bone
- 3. Bone Preparation – Damaged cartilage and bone are carefully removed using precision instruments
- 4. Prosthetic Placement – Metal components are fitted onto your femur and tibia; a plastic spacer is placed between them
- 5. Kneecap – Your surgeon may or may not replace the back of your kneecap (depending on arthritis severity)
- 6. Testing – Your surgeon checks that your knee moves smoothly through its full range
- 7. Closure – Incision is closed with stitches or staples
- a. Bandages applied
- b. Compression wrap to reduce swelling
- c. Your leg is elevated and supported
- d. You’re taken to recovery
Recovery: The Critical First 12 Weeks
1. Hospital Stay (1-2 nights)
- a. Pain management with medications
- b. Physical therapy begins (yes, the same day as surgery!)
- c. Blood clot prevention (compression stockings, blood thinner medication)
- d. You’ll be surprised—most people are walking with assistance the day after surgery
2. Weeks 1-2: Managing Pain and Swelling
- a. Intense swelling is normal (ice and elevation help)
- b. Pain is expected but manageable with medication
- c. Physical therapy 2-3 times per week
- d. Walking with a walker or crutches
- e. Sleeping in recliner or elevated position easier than lying flat
- f. Avoid driving
3. Weeks 3-6: Progressive Mobility
- a. Transition from walker to crutches to cane to no assistance
- b. Range of motion improves steadily (your therapist pushes you gently)
- c. Gentle weight-bearing exercises
- d. Pain decreases significantly
- Most people can return to light desk work
- Stairs become possible (with handrails)
- Driving might be possible (check with surgeon)
4. Weeks 6-12: Building Strength
- a. Range of motion is nearly normal
- b. Walking distances increase
- c. Quad and hamstring strengthening accelerates
- d. Balance training
- e. Stairs feel more natural
- f. Pain is minimal—mostly just stiffness
- g. Some people return to light activities
5. Months 3-6: Function and Confidence
- a. Most daily activities are pain-free and easy
- b. Walking becomes normal without thinking about it
- c. Swimming and water aerobics (excellent for strength without stress)
- d. Stationary cycling
- e. Light exercise
- f. Full range of motion achieved
6. Months 6-12: Return to Normal
- a. Low-impact activities feel normal
- b. Hiking, traveling, shopping without pain
- c. Sleeping normally
- d. Stairs without handrails
- e. Grandchild-chasing without limitation
- f. The prosthetic knee becomes “invisible”—you stop thinking about it
Rehabilitation: The Key to Success
Surgery is one day. Rehabilitation is 12 weeks (at minimum). Your success depends on:- 1. Physical therapy commitment – 3 sessions per week, minimum
- 2. Home exercises – Daily exercises (even when painful)
- 3. Patience – Recovery isn’t linear; some days are harder than others
- 4. Pain management – Using medication to allow you to participate in therapy
Cost of Knee Replacement in Hyderabad
Total knee replacement typically costs ₹2,50,000 to ₹4,50,000, depending on:- 1. Prosthetic brand (premium components cost more)
- 2. Hospital and surgeon reputation
- 3. Complexity of your case
- 4. Unilateral (one knee) vs. bilateral (both knees at once)
A. What’s Usually Included
- 1. Surgery and anesthesia
- 2. Hospital stay
- 3. Prosthetic components
- 4. Initial post-operative care
- 5. Follow-up visits (4-6 over 3 months)
B. What Might Be Extra
- 1. Physical therapy sessions (often separate from surgery cost)
- 2. Knee brace for post-operative support
- 3. Follow-up X-rays
C. The Long-Term Value
Yes, ₹2,50,000-4,50,000 is significant. But consider:- 1. Years of pain relief
- 2. Restored mobility
- 3. Ability to work and earn income
- 4. Ability to enjoy life with family
- 5. Average knee replacement lasts 15-20 years
How Long Do Knee Replacements Last?
Modern knee prosthetics are designed to last 15-20+ years. Some last 25+ years. This depends on:- a. Your activity level (higher activity = faster wear)
- b. Your weight (heavier people put more stress on prosthetics)
- c. Prosthetic quality (premium components last longer)
- d. Surgical technique
Risks and Complications
All surgeries have risks. But knee replacement complications are relatively rare.Common Temporary Issues
- 1. Swelling and bruising (expected)
- 2. Pain (manageable with medication and therapy)
- 3. Stiffness (resolves with physical therapy)
- 4. Blood clots (rare, prevented with medication and compression)
Less Common Complications
- 1. Infection (1-2%, treated with antibiotics or additional surgery)
- 2. Prosthetic loosening (10-15% after 15+ years, not immediately)
- 3. Persistent pain (2-10%, cause is often unclear, improves with time)
- 4. Patellar problems (if kneecap is replaced, can develop wear)
Life After Knee Replacement: What You Can Do
Activities You Can Do
- a. Walking (including hiking on easy trails)
- b. Swimming and water aerobics (excellent choice)
- c. Cycling (stationary or road, easy pace)
- d. Golf
- e. Bowling
- f. Gardening
- g. Traveling
- h. Climbing stairs
- Dancing (slow to moderate)
- Grandchild care without limitation
Activities to Avoid
- a. Running or jogging
- b. High-impact aerobics
- c. Basketball, volleyball, tennis
- d. Heavy contact sports
- e. Jumping
Making Your Decision
Knee replacement is a major decision. But for people who have struggled with arthritis pain, it’s often life-changing. Ask yourself:- a. Has pain limited my activities for 6+ months?
- b. Have conservative treatments not worked?
- c. Am I ready to commit to rehabilitation?
- d. Do I want my life back?
Your Next Step
Schedule a consultation with an orthopedic surgeon. They’ll:- a. Examine your knee
- b. Review X-rays and imaging
- c. Discuss your symptoms and lifestyle
- d. Explain whether you’re a good candidate
- e. Answer all your questions
- f. Discuss timing
Frequently Asked Questions About LASIK
Will I need pain medication forever?
No. After 6-12 months, most people take no pain medication. Some people never need it again.
Will I feel the prosthetic in my knee?
After a few months, most people forget it’s there. It becomes part of your body. Some people report occasional awareness (feeling “different”), but this usually resolves.
Can I fly after knee replacement?
Yes, usually after 4-6 weeks. Bring your surgical summary on flights (metal prosthetic might trigger security alarms).
Will I set off metal detectors?
Usually yes. Inform security officers. You’ll likely get a pat-down instead of going through the detector.
When can I drive again?
Usually 4-6 weeks if you’re off pain medication and have good range of motion. Your surgeon will clear you.
Can I have another knee replaced if needed?
Yes. If you need bilateral knee replacements, surgeons might do both at once or schedule them weeks apart (one leg heals while the other is rehabilitating).
Why Surgipatner
✔Right Doctor Guidance
✔ Best Hospitals in Your Budget
✔ Free Consultation
✔ Complete Surgery Support
What Our Patients & Partners Say
Posted onTrustindex verifies that the original source of the review is Google. I am thoroughly impressed with the SurgiPartner model, which delivers integrated, end-to-end patient support across the healthcare continuum—from initial consultations to treatment and surgical interventions, where necessary. I recently availed their Care Buddy service for a consultation, and the experience was highly seamless, efficient, and professionally managed. The structured Care Buddy support, combined with well-aligned financial assistance processes, significantly enhances the overall patient journey. This holistic and patient-centric approach effectively streamlines access to quality healthcare, making it more efficient and convenient in today’s dynamic environment.Posted onTrustindex verifies that the original source of the review is Google. I’m really impressed with the SurgiPartner concept. They provide end-to-end patient support—from doctor consultations to treatment and even surgery when required. I personally used their Care Buddy service for a consultation, and it was a smooth and positive experience. The Care Buddy assistance, along with support in financial processes, makes healthcare much more convenient, especially in today’s fast-paced lifestyle.Posted onTrustindex verifies that the original source of the review is Google. My Brother Arun Kumar and krishna from Bangalore. We are travelled to Hyderabad for LASIK surgery, and today we successfully underwent the procedure at American Laser Eye Hospital. The surgery went very smoothly and I am feeling very good after the procedure. The hospital environment is very clean and well maintained. All the staff and doctors are very polite, supportive, and professional. A special thanks to SurgiPartner CareBuddy for guiding and helping me throughout the entire process. From the beginning till the end of the day, they were with us at every step and provided excellent support. Overall, I had a very good experience and I highly recommend American Laser Eye Hospital for LASIK surgery with SurgiPartner support.Posted onTrustindex verifies that the original source of the review is Google. Really impressed with the concept of SurgiPartner. They offer complete patient support from doctor consultation to treatment and surgery if needed. I personally took a consultation through their Care buddy, and it was a great experience. The care buddy system and help with financial processes make healthcare much easier, especially in today’s busy world.Posted onTrustindex verifies that the original source of the review is Google. My name is Arun Kumar and I am from Bangalore. I traveled to Hyderabad for LASIK surgery, and today I successfully underwent the procedure at American Laser Eye Hospital. The surgery went very smoothly and I am feeling very good after the procedure. The hospital environment is very clean and well maintained. All the staff and doctors are very polite, supportive, and professional. A special thanks to SurgiPartner CareBuddy for guiding and helping me throughout the entire process. From the beginning till the end of the day, they were with us at every step and provided excellent support. Overall, I had a very good experience and I highly recommend American Laser Eye Hospital for LASIK surgery with SurgiPartner supportPosted onTrustindex verifies that the original source of the review is Google. Thank you for the support and service provided by SurgiPartner. The overall experience was smooth and the team was very helpful.Posted onTrustindex verifies that the original source of the review is Google. Staff is very good and nice receiving. They are very humble and their response is very good. Thank youPosted onTrustindex verifies that the original source of the review is Google. I want to thank Surgipartner for all the help and support during my LASIK surgery. From the beginning till the end, the team was very proactive with follow-ups and guided me clearly through every step, which made the whole experience easy and stress-free. I would especially like to appreciate CareBuddy Raju and Coordinator Anusha for their outstanding support. They were always in touch with both the hospital staff and me, helped reduce waiting time, and made sure everything went smoothly. Their care, quick responses, and constant guidance really made a big difference. Overall, I had a very positive experience and truly appreciate the support provided by Surgipartner.Verified by TrustindexTrustindex verified badge is the Universal Symbol of Trust. Only the greatest companies can get the verified badge who has a review score above 4.5, based on customer reviews over the past 12 months. Read more